- Home
- Services
- About
- News
- Contact
- Pills and potions remix
- Videoscribe videos
- Fnaf the twisted ones free pdf
- Rar unlocker online
- Risk 2 game download
- Gta 5 demo online free play
- Target w2k19
- Easy english short stories with big ideas
- Win7 service pack 1
- Serum osmolarity
- Howls moving castle movie eng sub
- Download borland c 64 bit windows 7
- Diy ecu flashing
- Mini cam belt
- Minecraft java edition
- Tekken 5 jin

Liver cirrhosis: Albumin is produced by the liver and then secreted out of the hepatic cells into the extravascular space, then returned to the blood via the lymphatic system. The proteinuria occurs when there is damage to the podocyte foot processes or the glomerular basement membrane, which results in decreased serum osmolality and oncotic pressure. Nephrotic syndrome: A general term that describes the disease processes which result in excessive loss of protein in the urine (proteinuria over 3 grams/day), accompanied by hypertriglyceridemia, hypoalbuminemia, and a hypercoagulable state. The treatment can involve medications that block the vasopressin receptor, such as tolvaptan, therapy with hypertonic saline, removing the medications inducing SIADH, or treating the primary cause. Syndrome of inappropriate antidiuretic hormone (SIADH): The condition occurs when the body produces an excessive amount of antidiuretic hormone (ADH) due to multiple causes such as central nervous system tumors, medications, and lung cancers, resulting in the kidneys reabsorbing too much water, which manifests as a dilutional hypoosmolar plasma and hypertension.

The final phase is water intoxication, manifesting as delirium, ataxia, nausea, seizures, vomiting, which may ultimately be fatal. First, polyuria and polydipsia, followed by the second phase as the kidney cannot excrete the excess water, resulting in hypoosmolar plasma that manifests as hyponatremia. Psychogenic polydipsia: A psychiatric condition characterized by self-induced water intoxication. For example, if a cell is in a relatively hyperosmolar solution, fluid will move out of the cell towards the highly concentrated compartment to reach homeostasis.
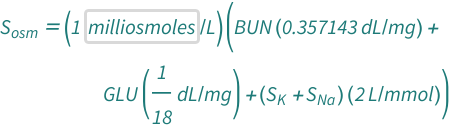
When water moves between plasma and intracellular compartments, the movement direction depends on both compartments' osmolalities.

Water normally flows from the compartment of low osmolality to the compartment of high osmolality this only occurs if the membrane between the two compartments is permeable to water. The normal serum osmolality should range from 275 to 295 mOsm/kg. Some authors argue that the formula 1.86(Na+K)+1.15(Glu/18)+(Urea/6)+14 is the most precise of them. Many other formulas have been developed and used over the years, but the simple Smithline-Gardner formula remains the most useful. concluded that the best formula was the simple Smithline-Gardner formula, where the plasma concentrations are measured in mmol/l. In 1976, Smithline and Gardner, proposed to use serum osmolality = 2(Na) + glucose/18 + BUN/1.8 as a simpler formula. The 1975 Dorwart and Chalmers formula, serum osmolality = 1.86(Na) + (glucose/18) + (BUN/2.8) + 9 had been often used to calculate the plasma osmolality. Specific therapies and toxins that affect an individual’s fluid balance should also be evaluated with serum osmolality. The blood urea nitrogen (BUN) measurement is important for calculating the serum osmolality. Serum osmolality is affected by the concentration of blood chemicals like chloride, sodium (Na), proteins, bicarbonate, and glucose. Serum and urine osmolality tests are usually measured together to be compared and reach the diagnosis of any disease that influences osmolality. It is routinely measured in clinical laboratories for the differential diagnosis of disorders related to the hydrolytic balance regulation, renal function, and small-molecule poisonings. Osmolality indicates the concentration of all the particles dissolved in body fluid.
- Home
- Services
- About
- News
- Contact
- Pills and potions remix
- Videoscribe videos
- Fnaf the twisted ones free pdf
- Rar unlocker online
- Risk 2 game download
- Gta 5 demo online free play
- Target w2k19
- Easy english short stories with big ideas
- Win7 service pack 1
- Serum osmolarity
- Howls moving castle movie eng sub
- Download borland c 64 bit windows 7
- Diy ecu flashing
- Mini cam belt
- Minecraft java edition
- Tekken 5 jin
